In early mornings along North King Street, a crowd of people lines up outside of Kalihi-Palama Health Center. If it’s raining, they’ll huddle beside the door for shelter. If it’s sunny, they’ll linger along the sidewalk, not speaking to one another, staring at their phones or the ground or watching the cars go by.
They’re waiting for the clinic to open at 7:45 a.m., and once it does, they’ll rush to enter. Some show up as early as 6 a.m., drawn by the promise of a relatively affordable clinic to fix the pain nagging their teeth. Many are immigrants who don’t speak English. Some are accompanied by relatives to help interpret.
The line in front of the clinic is a symptom of how hard it is to get oral health care in Hawaii if you’re already struggling to get by. The system isn’t set up to help low-income adults who need dental care.
On a recent Tuesday morning, Lee is among them. The 59-year-old drove from Pearl City an hour and a half ago to get a second opinion on whether he needs to pull out one of his left molars. He found parking, got a newspaper and waited anxiously for the clinic to open.
He’s there because a tooth on the left side of his mouth is hurting so badly that his dentist referred him to a specialist. But Lee, who is on Medicaid, said the specialist estimated it would cost $160 for a consultation, another $160 for an X-ray and more than $1,000 to reconstruct it.
“My doctor tells me, ‘Why don’t we just pull it out, save you some money,’” Lee said. “I’m 59 right now. If I pull it out, he says you can live with it.”

Nationwide, millions of low-income people lack access to dental insurance. Despite having a booming economy with only a 2 percent unemployment rate, Hawaii is no different.
The state cut Medicaid funding for non-emergency adult dental care services during the recession nearly a decade ago. That means Hawaii’s public health insurance for low-income people, Med-QUEST, won’t cover teeth cleanings, cavity fillings or even root canals. If you’re low-income and have a toothache, getting your tooth pulled out is often the only option.
Hawaii is among a minority of states that only fund emergency dental services for adult Medicaid patients. Four states don’t fund any dental services at all. Local health care providers and advocates for patients and people with disabilities urged the Legislature to reinstate the funding this year to no avail.
Gov. David Ige’s administration asked for $4.5 million in general funds and $6.5 in federal funds for the program this year. But Rep. Sylvia Luke, who chairs the House Finance Committee, said when she inquired with the Department of Human Services, she realized the program’s actual price tag was much steeper: $43 million annually, including $26 million in federal funds and $17 million in general funds.
Even if funding were appropriated, many dentists don’t accept Medicaid due to low reimbursement rates. A study of 2016 data found that when it came to children’s dental services, Hawaii had among the lowest Medicaid reimbursement rates relative to fees.
Advocates say funding non-emergency adult dental services is a necessary step to improving overall health and well-being for Hawaii’s low-income communities.

For Lee, the throbbing in his molar waxes and wanes but sometimes it’s so bad it wakes him up at night. It’s worse when he chews gum or eats steak. He wants to tell his story but he’s ashamed of how bad his teeth are and how he can’t afford to fix them. That’s why he refuses to provide his full name — Lee is his middle name.
Shame is a key part of America’s dental care crisis. The nation puts a premium on shiny, white teeth. They’re a sign of success and beauty whereas missing teeth are a source of humiliation, a visible symbol of poverty that may hinder people from getting jobs or pursuing opportunities to improve their situations. Shame is compounded by the challenges of working, sleeping, chewing, eating and talking when your mouth is in pain.
“I’m trying to save it but it just seems like whatever way I go to save my tooth it’s going to cost me big time,” Lee said. “I’d rather save my tooth but I can’t spend $1,500 to reconstruct that thing.”
Funding Slashed
Daniel Fujii, dental director at Waianae Coast Comprehensive Health Center, estimates adults in Hawaii have been without comprehensive dental coverage for more than two decades.
Funding for non-emergency adult dental services was cut in the mid-1990s, restored partially in 2006 and eliminated completely in 2009, Fujii said. “That’s a long time to be without assistance … We’ve got to take responsibility and not just wall it off (from other medical services).”
Dental services are funded differently from general health care because of a split in the medical profession that goes back more than a century, a separation that author Mary Otto chronicles in her book Teeth: The Story of Beauty, Inequality, and the Struggle for Oral Health in America.
The result in America is less resources and care for low-income communities. “The teeth are made from stern stuff. They can withstand floods, fires, even centuries in the grave,” Otto wrote. “But the teeth are no match for the slow-motion catastrophe that is a life of poverty: its burdens, distractions, diseases, privations, low expectations, transience, the addictive antidotes that offer temporary relief at usurious rates.”
David Derauf, a physician and director of Kokua Kalihi Valley Comprehensive Family Services, says cutting care for the mouth off of the rest of the body can have disastrous consequences.
“Why in the world would we treat this vital organ that sits next to the brain and the heart any differently?” he said. “It is absolutely essential to the pursuit of life liberty and happiness. It makes absolutely no sense that we segregate it.”

Untreated dental problems can lead to major illnesses, and even death. And society ends up bearing the burden through lack of worker productivity and costly emergency room visits.
States that cut adult dental care Medicaid benefits during economic downturns saw an increase in emergency room visits for oral health, Otto found. “The same financially stressed states and their taxpayers end up bearing the cost of deferred dental care in expensive emergency treatment for decay, abscesses, and other dental ailments anyway,” she wrote, citing the Pew Charitable Trusts.
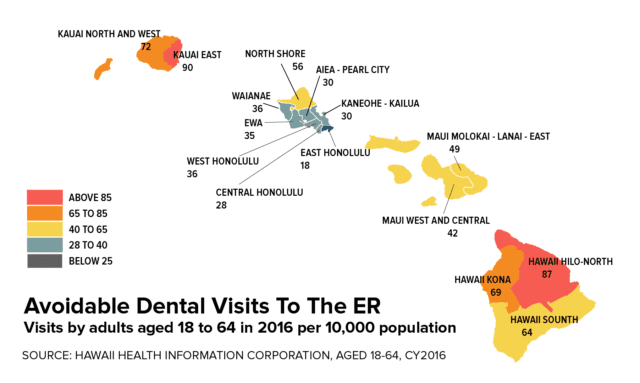
In Hawaii, there were nearly 5,000 emergency room visits related to dental problems in 2016 costing more than $6.6 million, according to data from the Hawaii Health Information Corp. That cost has more than doubled since 2007.
The data shows Med-QUEST patients make up more than half of ER visits related to dental care. They visited the ER for oral health problems less than 1,500 times back in 2007. In 2016, that number grew to more than 2,000, about twice as many visits as patients with private insurance.
Adults between the ages of 25 and 34 are most likely to use the ER for dental care. Each visit costs an average of $1,332, compared to $70 to $160 for a visit to the dentist. And the visits provide little relief.
“There’s not much they can do in the emergency room,” said Jill Miyamura, president of Hawaii Health Information Corp. “Either they’ll give you some drugs or they’ll pull the tooth. That’s basically it.”
The Human Toll
Even as he debates whether to pull out his tooth, Lee already can only chew on half of his mouth. When he was 28, he lost two teeth on the other half of his mouth after they got infected.
“I never bridged it, you know how much a bridge costs,” he said, estimating in the thousands. “So now it’s catching up with me.”
Three decades later, he says his upper tooth is sagging because there’s no lower tooth to connect with when he bites down. He thinks his left molar has been worn down from overuse.

In some ways, Lee is lucky. He lives in Honolulu, and if his visit to Kalihi-Palama doesn’t work out, he might be eligible to get care at the state’s only free dental clinic, Aloha Medical Mission, nearby at Palama Settlement. The organization relies on volunteer dentists to serve poor communities.
Services in rural areas are much harder to come by. Data from the Hawaii Health Information Corp. found residents of the North Shore of Oahu and neighbor islands are more likely than urban residents to go to the ER for oral health problems. That happens most often on Kauai and Hawaii Island.
There are racial and ethnic disparities too. Pacific Islanders, particularly Native Hawaiians, and African-Americans have the highest rates of ER visits for dental problems. The data shows Native Hawaiians visit the ER for dental care twice as often as people of Japanese or Chinese descent.
The cost of lack of dental care is more than just a dollar amount. Nationwide, toothaches lead to anxiety, lack of sleep and cause people to miss work. Missing or decayed teeth can hurt your chances of actually getting a job.
One study found that most people turn to prayer to deal with dental pain. Lee is no different. The night before coming to the clinic, he prayed hard. “Lord, I hope things work out right and if not, just protect me from everything.”
He thought of all the horror stories he had heard of dental problems gone wrong and wrestled with whether to create another gap in his mouth.
“Is it worth paying $1,500?” he wonders. “It’s kind of a stupid question but when you don’t have the money, it’s everything.”
No Dental School, No Fluoride In The Water
One way many communities seek to slow tooth decay is by adding fluoride to public water systems. But Honolulu actually banned doing so back in 2004.
Less than 12 percent of Hawaii public water contains fluoride compared to nearly 75 percent nationwide, according to 2014 data from the Centers for Disease Control and Prevention.
In other states, dental students may help provide services but Hawaii doesn’t have a dental school. The state also doesn’t have a dental public health program within the state Department of Health.
At the same time, Hawaii has the highest cost of living out of any state. Paying for dental care is harder when you’re struggling to afford the highest rents in the nation and your state is one of a minority that taxes food.
Luke said the lack of funding for adult dental care comes down to limited money and competing priorities.
Restoring preventative dental care funding for adults could cost $17 million per year, or more if Congress slashes funding for Medicaid. The Ige administration advocated for partial funding of the program this year but Luke says it didn’t make sense to fund just a portion of the need.
Luke said the Legislature will reconsider the issue next year. But $17 million is a lot of money for one program, she said, and there’s demand for the Legislature to fund other programs such as subsidies for caregivers.
Putting Up A Facade
When it comes to living in Hawaii, Lee knows he’s one of the lucky ones. He was born and raised here and inherited a home in Pearl City from his grandmother.
“Otherwise I’d be homeless,” he said. He works as a property manager and has a part-time job at the airport. He had to cut back his hours in recent years after getting sick. “I can hardly do my job — it’s real physical and I’m getting a little bit older.”
His physical health has gotten a lot better since he got on Medicaid nearly a decade ago. “Medicaid really helps me out because like I said I was really down and out (before I had it), now I get to see my doctors twice a year and that really, really, really helps.”
But dental care is different. Even if lawmakers decide to fund Medicaid next year, Lee knows it will be too late for him. He tries to stay positive though.
“If you look at me I’m kind of healthy, right, but the way things are in Hawaii, a lot of it is a facade,” he said. “You just know how to get through things.”
Thoughts on this or any other story? Write a Letter to the Editor. Send to news@civilbeat.org and put Letter in the subject line. 200 words max. You need to use your name and city and include a contact phone for verification purposes. And you can still comment on stories on our Facebook page.
 GET IN-DEPTH
REPORTING ON HAWAII’S BIGGEST ISSUES
GET IN-DEPTH
REPORTING ON HAWAII’S BIGGEST ISSUES
It's our job to make sense of it all.
The decisions shaping Hawaiʻi are happening right now, which is why it’s so important that everyone has access to the facts behind them.
By giving to our spring campaign TODAY, your gift will help support our vital work, including today’s legislative reporting and upcoming elections coverage.
About the Author
-
 Anita Hofschneider is a reporter for Civil Beat. You can reach her by email at anita@civilbeat.org or follow her on Twitter at @ahofschneider.
Anita Hofschneider is a reporter for Civil Beat. You can reach her by email at anita@civilbeat.org or follow her on Twitter at @ahofschneider.

