APIA, Samoa — As the sun set Thursday in Samoa, dozens of hungry and exhausted Hawaii health professionals ate dinner at a local hotel and retired to their rooms after a full day of mass vaccinations following a redeye flight from Honolulu.
For some it was their first meal of the day.
But just minutes away at the National Hospital of Samoa’s emergency department dedicated to measles patients, several critically ill children were being rushed in at about 6:30 p.m., says Robert Ruggieri.

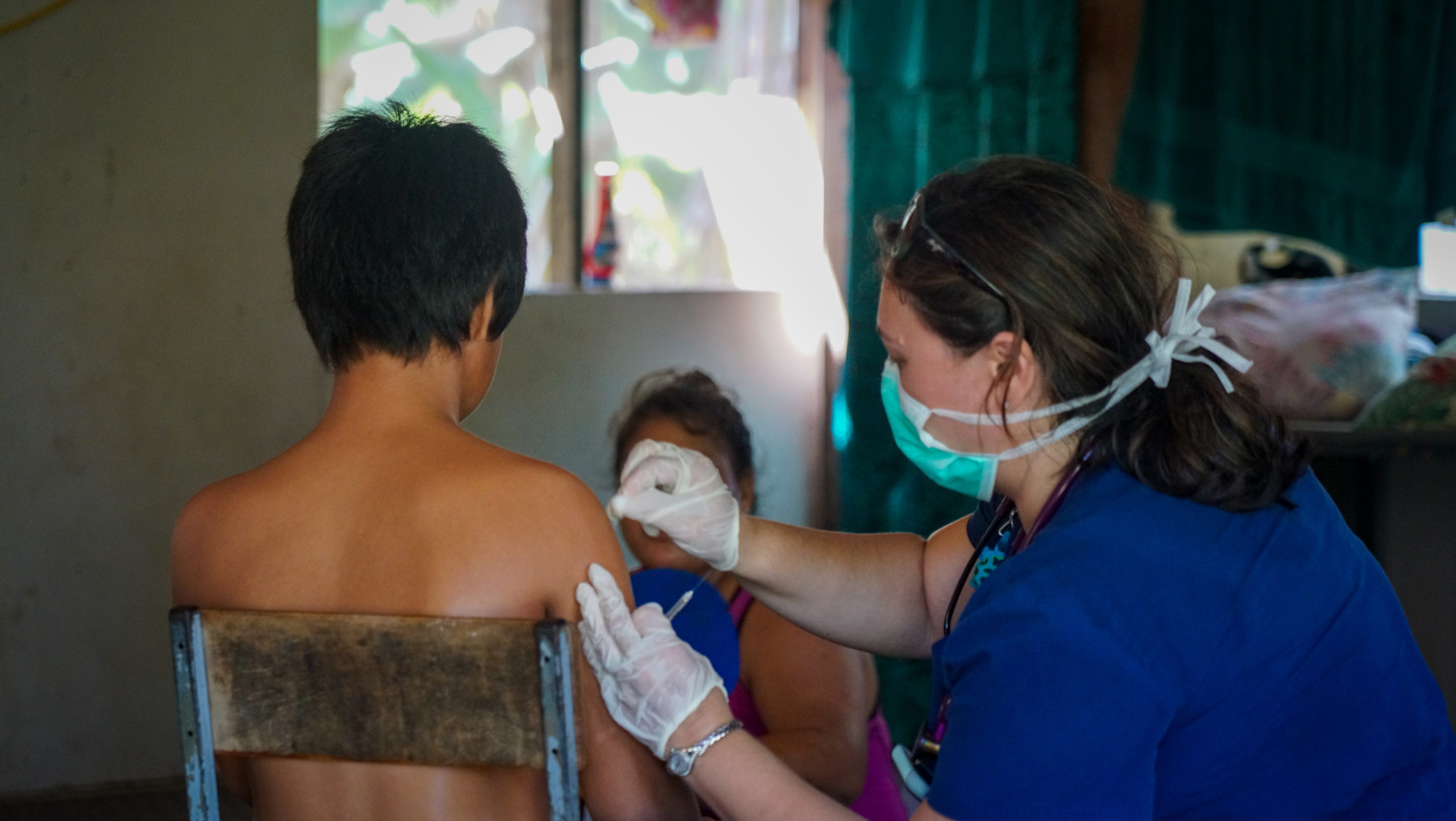
The Hawaii physician is among about 75 volunteers who flew from Hawaii to Samoa this week to help with the massive measles outbreak.
The country had been on lockdown all day — all residents except permitted personnel were ordered to stay home and off the roads while teams of vaccinators fanned out into the villages.
Within a couple hours after the curfew lifted, the hospital’s emergency room for measles patients was flooded with children mostly under the age of 2, Ruggieri says. He’s among a few Hawaii health care providers who volunteered at the hospital rather than go out into the field.

“They were really sick kids. They were underweight, they were severely dehydrated, they were lethargic and it was clear that most of them had pneumonia,” he said.
“They had all the symptoms of measles plus the complications of measles, so they had the pinkeye, the fever, the rash, they had been vomiting and had diarrhea and strometitis (inflamed mouth),” he said.
Ruggieri is an emergency room physician and founder of a popular string of urgent care clinics in Hawaii. But he felt in some ways out of his depth here in Samoa — the children were so dehydrated and young it was difficult and time-consuming to put IVs in their tiny veins.
By the end of the night, Samoa’s measles death toll ticked up to 63.
Transforming The Hospital
Friday — Thursday in Hawaii — was the second day of a medical mission by Hawaii doctors and nurses to help Samoa, part of a massive international effort to vaccinate 50,000 people and end the measles crisis.
More than 4,300 measles cases have been reported and most of the deaths have involved young children under the age of 4.
Twelve international teams are in Samoa this week to help both with immunizations and caring for sick patients. Nearly every division of the hospital is now dedicated to measles patients, says Sean Casey, who is working on the Samoa measles response for the World Health Organization.
“Suddenly the hospital which has all of these services became essentially one giant pediatric measles ward,” he says.
Within a couple hours after the curfew lifted, the hospital’s emergency room for measles patients was flooded with children mostly under the age of 2.
Because measles is airborne and highly contagious, it’s not easy to convert typical hospital rooms into contained rooms that prevent the spread of the disease. Some hospital divisions closed down entirely. The obstetrics ward split into two — one for pregnant women with measles and another designated as non-measles. Security guards are posted outside hospital doors to limit who can enter and exit.
One of the few non-measles wards is the former emergency department. That division went from seeing 40 to 50 patients per day to seeing more than 200 non-measles patients, but with a reduced staff because most of their staff were shifted to the hospital, says Casey.

The demand for measles-specific care is so high that teams from Australia even set up large air-conditioned, specialized tents outside the hospital to serve as contained wards. One tent with eight beds serves patients with critical conditions and is pressurized to limit the spread of disease. Two more large tents with another 20 beds were erected Wednesday.
Makeshift Resources
In an older yellow concrete building on one part of the hospital campus, rooms with signs for diabetes and other illnesses have been converted into a makeshift emergency center specifically for measles patients. Blue patterned curtains separate beds and a whiteboard lists names and ages of patients.
This is where Salote Vaai, a Samoan physician, has been working for the past couple of weeks. Vaai, a general practitioner who usually works in private practice, started helping with the government’s measles response two weeks ago.

Vaai is near the end of a nine-hour shift that started at midnight. Every day hundreds of patients come through this ward where she and other doctors stabilize them — giving them fluids if they’re dehydrated, offering pain relief and antibiotics if needed. Then they decide whether to send them home, hospitalize them or refer them to intensive care units.
It’s grueling work made harder by limited beds, staff and resources.
Related Stories
Pregnant women aren’t supposed to be in contact with measles, but she knows of some pregnant nurses who chose to work anyway because of the need.
In Vaai’s ward, she says they’re still missing special N-95 masks that resemble duck beaks and are better for protecting against airborne diseases.
She thinks those may be reserved for intensive care units. So instead they use regular masks that are less effective. Beds with IVs are limited too.
“What we’d like to do is offer everyone a bed and IV fluids and then send them home (if they don’t need more care). But we can’t, so what we do instead is we try to offer them fluids to try and drink and then send them home,” she said.

Over the last couple of weeks there’s been a huge influx of supplies and medical professionals to meet the demand.
When the outbreak first started, Samoa needed everything from ventilators to hand sanitizers. Countries like Australia and New Zealand — and now Hawaii — responded by flying large amounts of supplies to Apia. It’s made a huge difference and eased the biggest resource gaps, says Casey from the WHO.

Vaai said she’s so grateful for everyone and everything that’s arrived to help. She remembers one of her first days working in the emergency room when she and another doctor present were faced with two critically ill children.
“I was thinking, ‘How do we resus (resuscitate) these babies?’” she said, explaining usually there will be at least two people working on each resuscitation. She was so relieved when the hospital doors opened and a team of physicians from Australia poured in to help, a flood of blue uniforms that felt like an answered prayer.
Regaining Trust
The first child died of measles in Samoa on Oct. 13, a national holiday called White Sunday that celebrates childhood.
Taueu and Alesana Laumea were immediately afraid. They stopped letting their three daughters — a 5-year-old, a 2-year-old and an infant — go to school, playgrounds or family gatherings.
Their extended family organized to keep everyone healthy — Taueu’s brother was in charge of making icy mango and papaya juice smoothies for everyone every day.

But despite their best efforts, their youngest Shanella came down with measles in November, just days after turning 6 months old and receiving her first vaccination. They hadn’t realized she had already been infected.
At first they thought she was just feverish from teething. Then they saw her mouth sores and measles rash. For about a week she struggled with high fevers, often refusing to drink her bottle. Taueu’s mother vigilantly used a syringe to force her to stay hydrated, feeding her milk, mango juice and coconut juice.
Four days after her diagnosis, Shanella started getting better. But it felt like much longer than that to Taueu and Alesana. They know they’re among the lucky ones.
“When we look at our baby we feel like we are just so blessed,” Alesana says.

They don’t know personally the families who have lost children, but Taueu says throughout the community, “There’s a common feeling of sadness that’s just lingering.”
Fear still persists. Her 3-week-old nephew is not yet old enough to be immunized and remains on lockdown.
Taueu is so relieved that they had already vaccinated their two older daughters. The couple had hesitated before immunizing their 2-year-old — about two years ago, two children in Samoa died after nurses improperly mixed the measles vaccine. The investigation into their deaths took time and it wasn’t immediately clear that the children died due to human error.
When Taueu gave birth to their third daughter this year, they decided to move forward with their toddler’s immunization. “We were still worried but we wanted to make sure the girls were safe,” she says.
Now she says the vaccines prevented her older daughters from getting sick too. “I can speak from experience now that they work,” she said.
Vaai from the hospital says when the crisis is over, she wants to read an analysis of how it happened and why. But she knows it will be painful to see all the steps that should have been taken to prevent so many children from dying.
Anecdotally, she thinks that the crisis probably stems from multiple factors including child malnourishment, a low vaccination rate and a community where many see the hospital as a last resort, with some preferring to go first to traditional healers.
“We’ve lost a lot of trust between the public and the health system,” she said. “All those things together have kind of made us a sitting duck for something like this to happen.”
An Emotional Toll
Every day Vaai comes into the ward and reads the latest death count, looking up names to see if the children she cared for are among the dead. Just a couple days ago a baby died in an ambulance just 10 minutes before arriving at the hospital.
It’s sobering work, and isolating. She worries about what happens to the children that she sends away.
“We don’t always know the outcomes so that always weighs on us,” she says.
She doesn’t want to accidentally spread measles so she asked her siblings to keep her nieces and nephews away from her. The job also requires a lot of counseling for families.
“People just come in and they just say, ‘Oh I’ve just come to get the medicine for measles,’” she said. “We just have to try to explain to people that there is no medicine for measles.”
Still, she knows it’s harder for physicians working in the intensive care unit where every day they’re signing off on deaths and turning the machines off. Her eyes well up and redden as she describes the cascade of emotions that she and others are experiencing — disappointment, anger, regret, sadness.
But recently she’s started to feel hopeful. This week she’s seen fewer cases compared with last week, and the cases seem less dire. Someone even put up a couple of Christmas decorations in the ward, a couple of tiny balloons above the reception desk.
“I think everyone’s happy that it’s slowed down but I think everyone is just too paranoid to celebrate yet. So we are just waiting,” she said. “Hopefully it’s not a false lull.”
 Sign up for our FREE morning newsletter and face each day more informed.
Sign up for our FREE morning newsletter and face each day more informed.
It's our job to make sense of it all.
The decisions shaping Hawaiʻi are happening right now, which is why it’s so important that everyone has access to the facts behind them.
By giving to our spring campaign TODAY, your gift will help support our vital work, including today’s legislative reporting and upcoming elections coverage.
About the Author
-
 Anita Hofschneider is a reporter for Civil Beat. You can reach her by email at anita@civilbeat.org or follow her on Twitter at @ahofschneider.
Anita Hofschneider is a reporter for Civil Beat. You can reach her by email at anita@civilbeat.org or follow her on Twitter at @ahofschneider.



