“It feels a little like practicing medicine in a war and I am not ready for this …”
This was a statement from a very close friend, who is a family doctor in Canada. She was describing her anxiety around a treatment decision that required balancing concerns about bringing an older patient into her clinic for diagnosis and treatment of a chronic condition versus delaying standard care in order to reduce that patient’s risk of acquiring a COVID-19 infection.
Many of our doctors here are currently making similarly challenging treatment and management decisions. Almost no one is trained for this, emotionally or clinically.
As recently highlighted in an editorial in the Lancet, which is the world’s premier medical journal, health care workers are currently our most precious resource. They are at the frontlines of the pandemic and one of the groups most at risk of infection.
The risks taken by our health care workers are well-recognized, as is the unconscionable situation in which so many providers lack personal protective equipment, despite weeks of forewarning that a global pandemic was nearly inevitable.
Equally concerning is that health care workers can be a source of infection themselves, especially when they lack the equipment and support that would protect patients and other providers, and in a context in which it is still unclear how much transmission of COVID-19 occurs by asymptomatic individuals. There is no doubt that insufficient and maldistributed PPEs across the United States, and here in Hawaii, is an acute crisis that cannot be ignored.
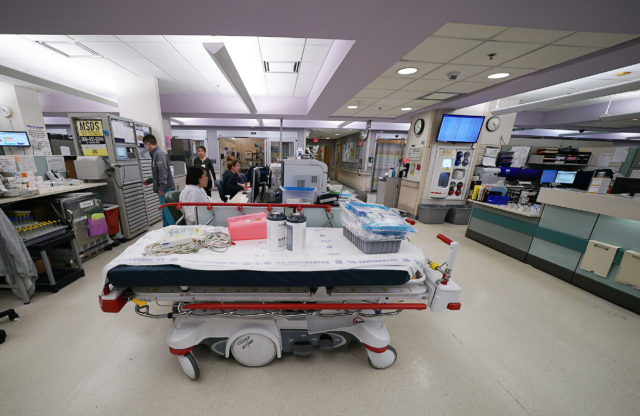
However, our providers need other forms of support too, including childcare and eldercare. With schools closed, like everyone else, our health care providers are balancing personal and professional roles and responsibilities.
Our heath care workforce is much larger than just doctors and nurses. It includes staff from a wide variety of disciplines (e.g., pharmacists, information technology specialists, laboratory technicians, interpreters, social workers, etc.) all of whom are critical to the proper functioning of our health system.
One group that is particularly vital, but frequently overlooked and under-celebrated, is custodial staff. In a context in which environmental cleaning and disinfection is paramount, both in and out of health care settings, assuring the health and wellbeing of our custodial staff should be among our highest priorities.
However, all health care staff at the moment need support, as the best way through this crisis is the full and coordinated mobilization of those who are trained to care for sick patients and their families.
While health care workers are our most valuable resource, our health system is currently our most valuable infrastructure. A health system is more than just hospitals. While definitions of health systems vary considerably by professional organization, generally speaking they encompass those that govern and guide health care decisions (policymakers and departments of health), entities that finance services (insurers, Medicaid and Medicare), as well as the places where services are delivered (hospitals, private practices, federally qualified health centers, etc.)
As the number of cases in Hawaii increases, all elements of the health system will be placed under incredible strain and if our local outbreak goes unmitigated, the system will collapse under the pressure.
Extreme Measures
It is crucial to consider what health system collapse looks like to better understand why such extreme measures have been taken to slow the spread of the virus. A collapsed health system entails much more than people with the virus, and resulting disease, not getting life-saving health care. That is, it entails more than being unable to get into an ICU or onto a ventilator when a sick patient needs one.
These are terrible consequences in-and-of-themselves and have been cited repeatedly as explanations for the high case-fatality rates in places like Wuhan, China, as well as in Italy and Spain. In these places, the health system could not keep up with demand.
A collapsed health system is much worse. It means that when car accidents happen, or heart attacks, patients are directly competing for care with those needing treatment for COVID-19 infection. Similarly, it means women who need cesareans to deliver or children with asthma attacks are also competing for care, as health personnel, equipment and materials are redirected towards managing the outbreak.
It means that health staff exhaust and burn out, compromising the quality of care their patients receive. It means that providers are forced to make decisions about who can or cannot receive life-saving care, decisions that may haunt them for years.
One group that is particularly vital is custodial staff.
As supplies for infection control dwindle, it means that care is provided under unsafe conditions for both patients and providers. The latter also means increased demands on a fragile health system as patients experience complications, such as secondary infections, and providers become sick and are removed from the workforce.
For all of us, it is imperative that we support all classes of health care workers and like many in the community already have, creatively seek solutions to the acute needs facing our health care staff (like insufficient PPEs).
Broader solutions for childcare and eldercare are also needed to assure frontline staff are able to focus fully on their jobs, knowing their loved ones are safe. As for the health care system, full mobilization of all resources under clear and undivided leadership is essential.
This last point is the most challenging, as the United States’ health care system is notoriously fragmented; nonetheless, it is probably the most essential for staving off some of the worst consequences of the outbreak.
 Sign up for our FREE morning newsletter and face each day more informed.
Sign up for our FREE morning newsletter and face each day more informed.
Community Voices aims to encourage broad discussion on many topics of community interest. It’s kind of a cross between Letters to the Editor and op-eds. This is your space to talk about important issues or interesting people who are making a difference in our world. Column lengths should be no more than 800 words and we need a current photo of the author and a bio. We welcome video commentary and other multimedia formats. Send to news@civilbeat.org. The opinions and information expressed in Community Voices are solely those of the authors and not Civil Beat.
What it means to support Civil Beat.
Supporting Civil Beat means you’re investing in a newsroom that can devote months to investigate corruption. It means we can cover vulnerable, overlooked communities because those stories matter. And, it means we serve you. And only you.
Donate today and help sustain the kind of journalism Hawaiʻi cannot afford to lose.



