Highly contagious variants of COVID-19 have become more prevalent in the islands even as the overall number of confirmed cases is on a downward trend, according to data released Wednesday by state health officials.
Of almost 1,500 specimens collected by the state laboratory since January, 1,023 were confirmed to be “variants of concern,” which have been flagged by federal health officials due to characteristics that cause an increase in transmissibility from the initial strain. The main ones were first discovered in California, the United Kingdom and Brazil.
“What makes them concerning is having a tendency to spread more quickly, which means they can be harder to contain, and also having more severe illness associated with them, like hospitalization and even death,” Dr. Sarah Kemble said Wednesday during a video press conference. “On the other hand, the good news is we’re still seeing more and more data come out that the vaccines available do work against these variants.”

Health authorities have been tracking the variants amid concern that they may pose a new threat to hopes that the state is on the road to recovery from the pandemic with growing momentum in the vaccination campaign and relatively low case numbers.
If new concerning variants emerge, they could prolong the pandemic or even outsmart vaccines.
“It is possible as the pandemic spreads and proliferates, variants could develop that have multiple mutations and are less responsive to the antibodies we form in response to the vaccine,” said Edward Desmond, the director of the Department of Health’s state laboratories division. “It’s possible we could need a booster vaccine in the future.”
Over time, viruses change and develop new genetic variations, each with its own characteristics. Some of those new attributes can allow the virus to spread with more ease, prompt severe disease or even evade immune response systems.
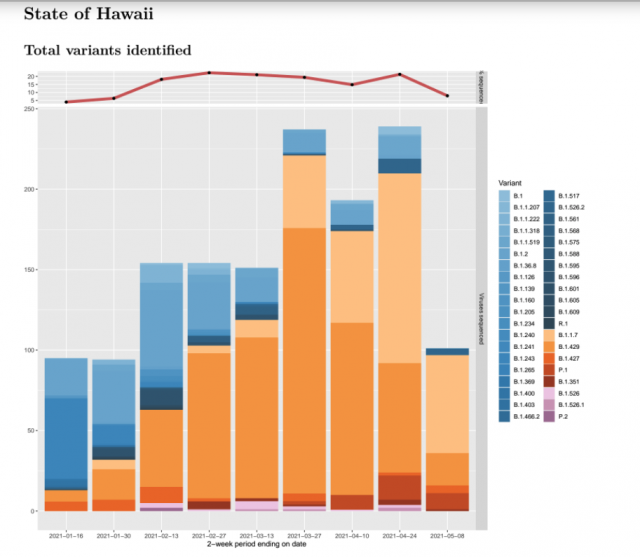
The main variant being found currently in Hawaii, known as B.1.1.7, originated in the United Kingdom and is estimated to be 50% more transmissible than the original dominant strain, and may cause more severe illness, based on hospitalizations and case fatality rates.
It surpassed the B.1.429 variant, which was first found in California and is believed by experts to be 20% more transmissible, in Hawaii in a span of three months, reflecting nationwide trends, officials said.
The P.1 variant, currently third most prevalent in Hawaii, was first detected in Japan and Brazil and could threaten the ability of antibody therapies currently available to treat patients. The Brazil and Japan variant is highly infectious and may be more resistant to antibodies. It was confirmed in 36 Hawaii test samples.
“We saw B.1.429 dominating then B.1.1.7 creeping up and taking over and we saw that trend mimicked here in Hawaii,” said Kemble.
Five variants of the SARS-CoV-2 virus, which causes the respiratory illness, are currently circulating throughout the United States.
Another variant that was first documented in India and remains behind the country’s devastating outbreak, has become dominant in the U.K. but has not yet been detected in the islands, Desmond said.
Current virus trends are stable in the islands, Desmond said. Hawaii saw an average of 50 new cases per day this week, and 1% of all tests conducted in the state during the last week were positive for COVID-19.
Still, variants and the possible future mutations they pose underscore the importance of vaccines, he said.
Diagnostic Laboratory Services, Inc. is among the local laboratories that archives COVID-19 test specimens in case they are needed by DOH for extra analysis.
The health department typically collects 75 specimens per week to do a full genomic analysis and determine whether or not they are new and emerging variations of the virus.
At the Department of Health’s State Laboratory Division in Pearl City, technicians assess specimens for the virus’ genetic information from a sampling of the Hawaii population, currently about 15% to 20% of all positives collected in the islands, according to Razvan Sultana, a bioinformatician at the DOH State Laboratories Division.
Ken Lincoln, the DLS laboratory’s director of communications, said more laboratories across the nation have joined the effort to conduct genomic sequencing.
DLS “stands ready to assist DOH should an expansion be desired,” Lincoln said in an email. “Thus far, this expansion has not been necessary in Hawaii because of our low positivity rate.”
Approximately half of Hawaii’s residents have been fully immunized against COVID-19. Kemble cautioned that the islands may still see outbreaks and masks will still be important to prevent transmission indoors.
Molokai, for example, has more than 50% of its residents fully vaccinated but saw a cluster of 16 infections associated with a hospital construction crew, she noted.
“We’re not yet at a point where we can’t see an outbreak,” she said. “I still think there’s going to be a role for wearing a mask indoors. That’s probably going to be the last thing to go.”
 Sign up for our FREE morning newsletter and face each day more informed.
Sign up for our FREE morning newsletter and face each day more informed.
What it means to support Civil Beat.
Supporting Civil Beat means you’re investing in a newsroom that can devote months to investigate corruption. It means we can cover vulnerable, overlooked communities because those stories matter. And, it means we serve you. And only you.
Donate today and help sustain the kind of journalism Hawaiʻi cannot afford to lose.
About the Author
-
 Eleni Avendaño, who covers public health issues, is a corps member with Report for America , a national nonprofit organization that places journalists in local newsrooms. Her health care coverage is also supported by the McInerny Foundation, the Atherton Family Foundation , the George Mason Fund of the Hawaii Community Foundation , and Papa Ola Lokahi . You can reach her by email at egill@civilbeat.org or follow her on Twitter at @lorineleni.
Eleni Avendaño, who covers public health issues, is a corps member with Report for America , a national nonprofit organization that places journalists in local newsrooms. Her health care coverage is also supported by the McInerny Foundation, the Atherton Family Foundation , the George Mason Fund of the Hawaii Community Foundation , and Papa Ola Lokahi . You can reach her by email at egill@civilbeat.org or follow her on Twitter at @lorineleni.

