Fear of contracting the new coronavirus is causing people across Hawaii to delay medical procedures, skip doctor visits and avoid hospitals.
Mia Taylor, director of community and post-acute care services for the Queen’s Health Systems, said a concerning number of patients are canceling or postponing preventative care procedures, such as physical exams, mammograms and colonoscopies.
People are also taking serious risks by neglecting important features of chronic disease management like eye exams, echocardiography and diabetic foot exams.
“We’re super worried about this because we just feel like it could be the next pandemic or tsunami, if you will, of people who have put aside some of these very important evaluations,” Taylor said. “As a result we feel like we may see this big uptick in complications associated with chronic disease.”
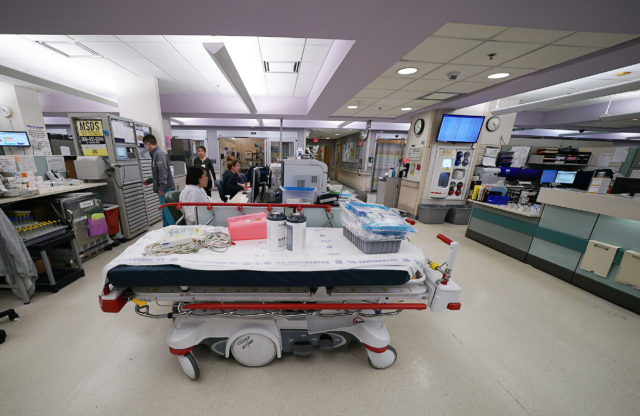
Many facilities halted non-emergency procedures when the virus invaded Hawaii in March. This month, with fewer new COVID-19 cases confirmed daily, many hospitals across the state are starting to bring them back.
But health care workers say some patients are continuing to defer medical care.
Hospital executives say the revenue usually generated by these non-emergency services has dipped significantly. And with some patients still too leery of the virus to visit a medical facility, it’s unclear when this revenue shortfall will recover.
“We’re doing a big radio, TV, and newspaper ad campaign announcing that we are open for business,” Taylor said. “This hospital is cleaner now than it’s ever been just with all the new CDC guidance, and we are doing everything we can to keep patients and staff safe.”
Health care providers are concerned that patients may be taking serious, potentially life-threatening risks by delaying treatment and preventative care.
In one case, Taylor said a patient who refused to seek medical care outside his home called his physician because he wasn’t feeling well and thought he might have a urinary tract infection. The physician prescribed antibiotics.
Later on, a worried family member called the physician to say that the patient still seemed very ill but could not be convinced to go to the emergency room.
A nurse was sent to the patient’s home and ended up having to call 911. The patient had a potentially life-threatening infection.
“The primary care doctor felt very strongly that had we not intervened when we did the patient would have died,” Taylor said.
Emergency room visits are also down statewide, with Maui Memorial Medical Center reporting a 50% drop in ER visits in April and so far in May when compared to the same period last year.
The Maui hospital was the site of the state’s largest COVID-19 cluster outbreak, which state health regulators say is now considered closed. All told, 38 health care workers and 14 patients were infected in the cluster.
The outbreak raised public safety concerns after staff interviewed by Civil Beat said the hospital was slow to require health care workers to wear personal protective equipment and also told some staff not to wear it.
An investigation by state health officials concluded that the outbreak appears to have been started by a hospital staff member who was allowed to work while feeling sick.

Health officials say plummeting ER traffic across Hawaii is partly owed to the fact there have been fewer accidents and injuries while many people have been sequestered at home. But they acknowledge that other patients are ignoring even severe mental health and medical symptoms because they are frightened to enter a hospital or doctor’s office.
ER traffic is also down by about half at Kauai Veterans Memorial Hospital and Samuel Mahelona Memorial Hospital, where Dr. Travis Parker, the emergency room medical director, said some people are staying away from the ER out of a “sense of duty.”
“I see a lot of people who come in with emergency-worthy symptoms and they apologize, ‘Oh I’m sorry I’m here taking up your time,’ because they perceive that we are so busy dealing with COVID,” Parker said. “They think they’re doing their part by not coming in.”
Dr. Laura DeVilbiss, medical director at Kokua Kalihi Valley, said one of her patients didn’t want to come into the clinic so she met her virtually with telemedicine for a follow-up appointment. The patient was doing fine at the time, DeVilbiss said.
But later in the day the patient developed symptoms consistent with a heart attack.
“When she knew she was having a heart attack, she went right to the ER,” DeVilbiss said. “I think people are going when they really, really need to, at least that’s what we’re hoping.”
People who rely on public transportation have also been resistant to coming into the clinic, she said, because they didn’t want to get on a bus — especially in March and April when the risk of exposure to the virus was higher than it is now.
Dr. Annie Nguyen, a psychiatrist in Kailua, said she has seen an uptick in patients who are adamantly refusing to seek urgent medical care.
When she can’t convince them to go to the hospital, she tries to persuade them to visit their primary care provider. When all else fails, she urges them to at least see a doctor through telemedicine.
“I try to stay in my scope because I can’t tell if someone has a broken foot,” Nguyen said. “But it’s obvious if someone can’t breathe or they’ve got a bone sticking out or they’re bleeding profusely that they need to get to the ER right away and getting people to go during the pandemic is sometimes a struggle.”
Suicide, Coronavirus Fears Lead To ‘Double Crisis’
By contrast, doctors say hospital admissions for psychiatric problems are up at some Hawaii facilities as the economy unravels and many feel isolated by public health restrictions.
Yet at the same time, some people in the throes of a mental health crisis, including those who are suicidal or who have overdosed, are showing a reluctance to seek emergency care due to COVID-19 fears.
Dr. Tanya Gamby, a psychologist on Kauai, said three of her patients who are suicidal have refused to go to the emergency room since mid-March.
One of those patients, she said, was in urgent need of emergency medical attention. Gamby said she ended up having to call the police, who showed up and insisted that this person go to the ER.
“It was definitely scary as a mental health professional knowing our procedures were not really working because nobody wanted to go to the hospital — and I wasn’t really wanting to send anyone there either,” Gamby said. “It felt like I had a double crisis on my hands.”
The other two patients who refused to go to the ER were not in active crisis, Gamby said. Out of concern, she said she provided them with extra therapy and more frequent check-ins.
Dr. Adrianna Flavin, a psychologist on Maui, said some of her suicidal patients have similarly expressed an unwillingness to go to the ER until the risk of contracting COVID-19 subsides.
“There was at least one person over the last two months where I’ve said to them, ‘If you are suicidal and you do develop a plan, I want to strongly encourage you to go to the hospital. It will be really important,’ and they said, ‘Oh, absolutely not,’” Flavin said.
“They won’t do it and they were telling me that upfront. And it was only because of the virus that they wouldn’t go.”
Boosting Health Care At Home
In many cases, there’s no suitable stand-in for in-person medical treatment.
But telemedicine can sometimes be a useful substitute for patients who need to see a doctor and are unwilling or unable to leave their homes.
However, not everyone has access to the technology that telemedicine requires: a computer, tablet or smartphone and a steady internet connection. Others might have this technology but don’t know how to use it.

Some providers have been visiting patients in their homes during the pandemic to teach them how to use telemedicine. Others have resorted to talking with patients over the telephone.
In some households, tech-savvy children who are home from school are providing their parents and grandparents with readily available tech support.
At Queen’s Health Systems, a new team is working to figure out how to augment telemedicine with self-monitoring tools like blood pressure cuffs, scales, thermometers and pulse oximeters. For people with chronic conditions, consistent monitoring of these vital signs can be critical.
The medical group recently partnered with the American Heart Association to distribute 80 bluetooth-enabled blood pressure cuffs to chronic disease patients so they can monitor key vital signs and discuss them with a doctor without leaving their home.
“It’s not ideal obviously for people with chronic conditions,” Taylor said. “Many of them were used to seeing their doctor every one to two months. But it’s definitely, I think, a viable surrogate until we can really get patients comfortable coming back in to their providers.”
Want more information on COVID-19 in Hawaii? You can read all of Civil Beat’s coronavirus coverage, find answers to frequently asked questions or sign up for email newsletter updates — all for free. And check out pictures of how community groups and volunteers have been helping out in our Community Scrapbook.
 Sign up for our FREE morning newsletter and face each day more informed.
Sign up for our FREE morning newsletter and face each day more informed.
What it means to support Civil Beat.
Supporting Civil Beat means you’re investing in a newsroom that can devote months to investigate corruption. It means we can cover vulnerable, overlooked communities because those stories matter. And, it means serve you. And only you.
Donate today and help sustain the kind of journalism Hawaiʻi cannot afford to lose.


